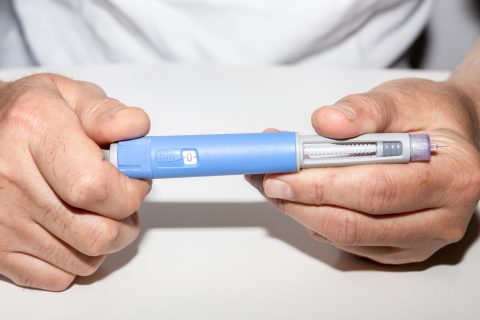
Byetta (exenatide)
Byetta (exenatide) is a discontinued diabetes drug linked to rare but serious side effects like pancreatitis, kidney problems and potential pancreatic cancer. The U.S. Food & Drug Administration (FDA) has issued multiple safety warnings, while Byetta lawsuits accused manufacturers of failing to warn about these risks.
Our content is developed and backed by respected legal, medical and scientific experts. More than 30 contributors, including product liability attorneys and board-certified physicians, have reviewed our website to ensure it’s medically sound and legally accurate.
legal help when you need it most.
Drugwatch has provided people injured by harmful drugs and devices with reliable answers and experienced legal help since 2009. Brought to you by The Wilson Firm LLP, we've pursued justice for more than 20,000 families and secured $324 million in settlements and verdicts against negligent manufacturers.
More than 30 contributors, including mass tort attorneys and board-certified doctors, have reviewed our website and added their unique perspectives to ensure you get the most updated and highest quality information.
Drugwatch.com is AACI-certified as a trusted medical content website and is produced by lawyers, a patient advocate and award-winning journalists whose affiliations include the American Bar Association and the American Medical Writers Association.
About Drugwatch.com
- 17 Years of Advocacy
- $324 Million Recovered for Clients
- 20,000 Families Helped
- A+ BBB Rating
- 4.9 Stars from Google Reviews
Testimonials
I found Drugwatch to be very helpful with finding the right lawyers. We had the opportunity to share our story as well, so that more people can be aware of NEC. We are forever grateful for them.
- Medically reviewed by Jessica Swirble, PharmD
- Last update: May 8, 2026
- Est. Read Time: 6 min read
What Is Byetta?
Byetta (exenatide) was an injectable medication prescribed to manage blood sugar levels in adults with Type 2 diabetes. Its active ingredient is exenatide, and it belongs to the glucagon-like peptide-1 (GLP-1) agonist drug class.
The medication was designed to be used alongside a diet and exercise program. It can be combined with other diabetes drugs.
- Lowers sugar production by your liver
- Makes your pancreas produce more insulin when your blood sugar is high
- Reduces your appetite
- Slows down the movement of food from your stomach to your intestine, which slows down sugar absorption
The medication was available in prefilled pens with standard microgram dosages of five mcg or 10 mcg per injection. It was taken twice daily before meals.
What Is Byetta Approved To Treat?
Byetta was FDA-approved for Type 2 diabetes management, not Type 1 diabetes. While it may contribute to modest weight loss for some people, it was not approved or typically prescribed for weight loss.
Newer GLP-1 drugs, including Ozempic (semaglutide) and Mounjaro (tirzepatide), have been prescribed for off-label purposes not approved by the FDA, including weight loss. Other diabetes drugs, like Wegovy (semaglutide) and Saxenda (liraglutide), are FDA-approved for weight loss.
Byetta Side Effects
Common side effects of Byetta, including nausea, indigestion and vomiting, are typically mild and go away after your body adjusts to the medication. Byetta may also cause serious side effects such as pancreatitis (inflammation of the pancreas).
“The most common side effects people notice [with GLP-1 medications] are going to be things like nausea, upset stomach, constipation, acid reflux, and sometimes vomiting and diarrhea, especially when first starting the medicine or increasing the dose,” Dr. Lauren Cunningham told Drugwatch.
- Constipation
- Diarrhea
- Dizziness
- Feeling jittery
- Headache
- Indigestion
- Nausea
- Vomiting
- Weakness
To avoid common side effects, doctors started people at a lower dose and slowly increased it over time, Cunningham said. These side effects will usually go away after a few days or weeks.
If they bother you or don’t go away, talk to your medical provider.
“The most common side effects people notice [with GLP-1 medications] are going to be things like nausea, upset stomach, constipation, acid reflux, and sometimes vomiting and diarrhea.”
Serious Byetta Side Effects
While most people will only experience mild side effects, Byetta can have serious side effects that may affect your pancreas, kidneys and digestive tract. These severe side effects may require additional treatment.
- Acute pancreatitis (inflammation of the pancreas)
- Allergic reactions
- Food or liquid getting into the lungs during surgery that requires anesthesia
- Gallbladder problems
- Kidney injuries caused by dehydration
- Low blood sugar
- Severe stomach problems (not recommended for people with gastroparesis)
Because acute pancreatitis can be a precursor to pancreatic cancer, it is possible that Byetta and other GLP-1 drugs could increase your risk of pancreatic cancer. However, most studies haven’t found an increased pancreatic cancer risk.
Acute Kidney Injury
In rare cases, patients who took Byetta have experienced impaired kidney function that can lead to kidney failure. Symptoms of kidney injury may include persistent nausea, vomiting and diarrhea that does not improve over time.
Notify your doctor if these symptoms last for more than a few days or if you have trouble taking liquids by mouth. These issues could put you at an increased risk of kidney problems.
“Byetta may cause new or worse problems with kidney function, including kidney failure. Dialysis or kidney transplant may be needed.”
According to a 2022 study published in Frontiers in Endocrinology, the risk of acute kidney injury is higher in patients taking liraglutide compared to exenatide, the active ingredient in Byetta.
However, anyone with a history of kidney disease should carefully consider the risks of kidney failure associated with any GLP-1 receptor agonist drugs.
Pancreatitis
The Byetta label includes a warning about an increased risk of hemorrhagic or necrotizing pancreatitis. This is a condition involving inflammation of your pancreas that can become fatal.
Chronic pancreatitis can cause permanent damage to your pancreas. Symptoms include abdominal pain, upset stomach, fever and weight loss. If you have a history of pancreatitis, an alternative antidiabetic medication might be a safer choice.
If you notice any of these symptoms while taking Byetta, you should consult a medical professional to see if you need to discontinue the medication. You should not stop taking your medication without your doctor’s approval.
Most Recent Byetta Side Effects Information
As of October 2025, the most common Byetta side effects reported to the FDA were hyperglycemia, weight loss, low blood sugar and gastrointestinal upset (nausea, vomiting and diarrhea). These symptoms are often mild, but changes to your blood sugar levels can become serious.
Dizziness and headache were additional mild side effects reported frequently to the FDA. Pancreatitis, while not common, happens often enough to appear in the FDA’s Adverse Events Reporting System (FAERS). Byetta’s packaging includes a warning about the risk of developing pancreatitis and pre-cancerous pancreatic cells.
| FDA Adverse Events Reporting System (FAERS) Data for Byetta, Exenatide and Exenatide Synthetic Side Effects | |
|---|---|
| Total cases reported | 79,267 |
| Serious cases (including deaths) | 17,758 |
| Deaths | 1,965 |
Disclaimer: Reports sent to the FDA don’t necessarily mean the drug caused an adverse event. Consult a health care professional before stopping or changing medication.
The annual number of adverse effects reported to the FDA for Byetta has decreased steadily since 2019. Among the millions of Byetta prescriptions written since 2005, fewer than 80,000 total cases have resulted in adverse events.
However, it’s important to note that about 22% of reported Byetta cases have involved serious side effects. If you have concerns about taking Byetta, talk to your doctor about the benefits and risks.
What Does Science Say About Pancreatic Cancer?
The science behind serious Byetta side effects like pancreatitis and pancreatic cancer is mixed. Many studies didn’t find a link to pancreatic cancer.
In 2013, the FDA issued a safety warning about unpublished findings linking GLP-1 drugs, also called incretin mimetics, to pancreatitis and pre-cancerous cells in the pancreas.
This warning also referenced a published study that suggested Byetta use could double the risk of developing acute pancreatitis.
-
2007
Label updated with a warning about acute pancreatitis.
-
2009
FDA warning for renal failure.
-
2013
FDA safety communication reviewing data on pancreatic cancer risk.
-
2021
FDA required an updated warning about the risk of hypoglycemia in patients using Byetta in combination with insulin or other drugs that increase insulin levels.
Since the initial FDA warning in 2013, more studies have come out that don’t show an increase in pancreatic cancer. For example, a 2024 study published in JAMA found no increased incidence of pancreatic cancer in 543,595 people who took a GLP-1 drug over seven years.
The FDA also hasn’t found evidence that Byetta and other GLP-1s cause pancreatic cancer.
In 2021, the FDA also required an updated warning about the risk of hypoglycemia, including severe hypoglycemia, in patients using Byetta in combination with insulin or other drugs that increase insulin levels. Patients should be made aware of the risk and the warning signs of severe hypoglycemia before taking Byetta.
Byetta Lawsuits and Legal Controversy
The initial FDA GLP-1 pancreatic cancer warning in 2013 led many people to file Byetta lawsuits as well as lawsuits against the makers of other diabetes drugs like Janumet, Januvia and Victoza. According to the plaintiffs, these drugs caused them to develop pancreatic cancer, and they weren’t warned about the risk.
- Failure to warn: No adequate warning about pancreatic cancer risks.
- Negligent misrepresentation: Alleged minimization of risks in marketing.
In 2013, these lawsuits were grouped together in one large litigation called a multidistrict litigation (MDL). In an MDL, similar claims against the same defendants are consolidated to make litigation more efficient.
-
2013
Hundreds of cases consolidated into Incretin Mimetics MDL No. 2452.
-
2015
Judge Anthony J. Battaglia dismissed failure-to-warn claims based on preemption. The Court found that there was enough evidence to show that the FDA wouldn’t have approved a pancreatic cancer warning.
-
2017
The Ninth Circuit Court of Appeals revived portions of the litigation.
-
2021
After more discovery, Judge Battaglia dismissed claims based on preemption again.
Ultimately, the MDL litigation ended in 2021 after the cases were dismissed for good.
What This Means for Patients
The good news for patients is that newer studies haven’t found that Byetta increases pancreatic cancer risk. However, the drug still has a warning for pancreatitis. Patients should discuss the risks and symptoms of pancreatitis with their doctor.
Even though pancreatic cancer litigation involving GLP-1 drugs is pretty much over, newer GLP-1 drugs face recent lawsuits for severe stomach problems and a rare vision disorder called NAION.
For example, Ozempic lawsuits say the drug can cause stomach paralysis as well as NAION vision loss. There are similar claims in Wegovy, Saxenda and Victoza lawsuits.
Calling this number connects you with a Drugwatch.com representative. We will direct you to one of our trusted legal partners for a free case review.
Drugwatch.com's trusted legal partners support the organization's mission to keep people safe from dangerous drugs and medical devices. For more information, visit our partners page.




