IVC Filter Complications, Lawsuits and FDA
IVC filters are medical devices designed to prevent life-threatening blood clots from reaching your lungs. However, several brands of IVC filters have been linked to serious injuries, recalls, regulatory scrutiny and lawsuits.
Our content is developed and backed by respected legal, medical and scientific experts. More than 30 contributors, including product liability attorneys and board-certified physicians, have reviewed our website to ensure it’s medically sound and legally accurate.
legal help when you need it most.
Drugwatch has provided people injured by harmful drugs and devices with reliable answers and experienced legal help since 2009. Brought to you by The Wilson Firm LLP, we've pursued justice for more than 20,000 families and secured $324 million in settlements and verdicts against negligent manufacturers.
More than 30 contributors, including mass tort attorneys and board-certified doctors, have reviewed our website and added their unique perspectives to ensure you get the most updated and highest quality information.
Drugwatch.com is AACI-certified as a trusted medical content website and is produced by lawyers, a patient advocate and award-winning journalists whose affiliations include the American Bar Association and the American Medical Writers Association.
About Drugwatch.com
- 17 Years of Advocacy
- $324 Million Recovered for Clients
- 20,000 Families Helped
- A+ BBB Rating
- 4.9 Stars from Google Reviews
Testimonials
I found Drugwatch to be very helpful with finding the right lawyers. We had the opportunity to share our story as well, so that more people can be aware of NEC. We are forever grateful for them.
- Medically reviewed by William T. Kuo, M.D., FSIR, FCCP, FSVM, FCIRSE
- Last update: April 10, 2026
- Est. Read Time: 14 min read
What Are IVC Filters and What Can Go Wrong?
Inferior vena cava (IVC) filters are small devices that are implanted in the large vein that carries blood from your lower body to your heart. They’re used in patients at risk for pulmonary embolisms who can’t take blood thinners.
While some filters are designed to be temporary, many are left in the body longer than intended. According to the U.S. Food and Drug Administration (FDA), leaving them in for more than a few weeks increases the risk of complications like IVC perforation or migration.
- Permanent filters: For patients who cannot take long-term anticoagulation treatments.
- Retrievable filters: Designed for temporary use, though studies show only 15% are removed.
“There are probably over two dozen filter types floating around in the U.S. Some are old, permanent ones that have been discontinued. All the way to the latest ones that have been released,” Dr. William Kuo, Director of the Stanford IVC Filter Clinic, told Drugwatch. The clinic pioneered new methods for removing IVC filters that have been left in the body for extended periods.
Types of IVC Filter Complications
IVC filter complications vary but can include breakage, deep vein thrombosis, pain and more. They are categorized by type, with certain complications overlapping into multiple categories.
- Complications from Placement
- Deep Vein Thrombosis (DVT)
- Defects
- Delayed Symptoms
- Detachment
- Immediate Symptoms
- Pain
- Tilting, Breakage and Migration
Dr. Kuo helped pioneer the field of advanced IVC filter retrieval, including the use of an excimer laser to remove embedded devices that cannot be safely removed using standard methods. He and his team at Stanford have performed thousands of advanced filter retrievals.
“I see the whole spectrum of IVC filter complications — filter components can penetrate through the vein and cause pain, while some pieces can break, migrate and cause other problems. An old filter can also cause scarring in the vein leading to vessel occlusion, debilitating leg pain with swelling and greater risk for blood clots,” Dr. Kuo told Drugwatch.
“Even if patients have not yet suffered these complications, the knowledge that they could develop in the future creates real anxiety among these patients,” he said.
Complications Can Cause Immediate Symptoms or Be Delayed
Depending on the type of complication, you may experience no immediate symptoms. Alternately, you may develop immediate pain or severe problems years later. In some instances, the side effects can be painful and dangerous.
“It’s like a knife being pushed into your stomach,” one patient told a television reporter, explaining the experience of having her IVC filter twist and puncture the walls of the vessel where it had been implanted three years earlier.
Clare Austin of South Florida said surgeons had to make an incision of approximately 10 inches in her belly to remove the filter.
“When I woke up I was in horrendous pain. A few days later when I finally saw the incision … that was unbelievable.”
If your filter has been implanted for several years, you should consult your doctor to assess the status of your device. Evaluations with routine X-rays or a CT scan might be warranted.. If there is any uncertainty regarding possible complications, then your case should be reviewed by a specialist.
“For patients with an indwelling device, it is important to check in with a physician who can at least identify what type of device was implanted. Recent X-rays should be reviewed to identify the filter type, assess for filter integrity and examine for other complications. A specialist can also help determine the need and feasibility of potential removal versus ongoing follow-up,” Dr. Kuo said.
Newer techniques have been developed that allow most filters to be removed using minimally-invasive methods (small < 1 cm incision) with quick recovery times, avoiding the need for large, painful incisions or open vascular surgery.
Serious Injuries Possible if IVC Filters Remain in for Too Long
The FDA warns that the risk of serious complications, including filter fracture, filter-associated IVC thrombosis or vein perforation, increases significantly when retrievable filters remain in place for more than 29 to 54 days.
- Filter fracture or migration: Filters can break apart or travel to your heart or lungs, causing an embolism.
- Filter-associated IVC thrombosis: A blood clot may get trapped in your filter, leading to pain, edema, ulcers and more.
- Increased deep vein thrombosis (DVT) risk: DVT happens when a blood clot forms in your deep veins, typically in your legs. This can cause pain or swelling in your leg.
- Vein perforation: Your filter’s legs may penetrate your IVC walls, causing damage.
Device fracturing has long been a concern with IVC filters. A 2012 Journal of Interventional Radiology study found that 40% of Bard filters left in place for 5.5 years fractured.
“Historically, most filters that have been implanted in the U.S. have not been adequately followed [by doctors] for possible removal,” Dr. Kuo shared.
He warns that if doctors do not follow up with these patients for potential complications or removal, the filters may become stuck for years. This may lead to complications.
“By then, it can be a real challenge to take these filters out,” Dr. Kuo said.
Complications from Placement
Major complications related to filter insertion happen less than 1% of the time. Most complications are minor and include small bleeding or a small blood clot at the access site.
Rarely, there may be accidental puncture of an adjacent artery. Some patients may develop an infection at the insertion site.
Short-Term Placement Complications
Possible procedural risks include the guide wire penetrating your vein as well as bleeding, clots or infection of the insertion site. You may also develop reactions to the contrast agent used during the procedure that can lead to kidney dysfunction, but this is rare.
A rare complication is the formation of an arteriovenous fistula, which involves an abnormal connection between an artery and a vein. The reported incidence of this complication is 0.02%.
As with most procedures that are done through the skin, filter placement also carries the risk of developing a collapsed lung (pneumothorax) or a collection of blood in between the chest wall and lung (hemothorax).
Other complications can include the accidental introduction of air into a blood vessel, called an air embolus, and heart rhythm abnormalities.
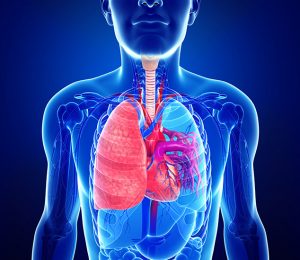
Doctors place IVC filters to stop blood clots from traveling to your lungs.
Access Site Bleeding and Misplacement
The rate of bleeding at the access site is estimated between 6% and 15%. Significant bleeding that would require a transfusion or surgery is rare.
You can also develop blood clots at the insertion site. This is more common if you are hypercoagulable, meaning you have blood that tends to clot too much.
In rare instances, medical professionals have incorrectly oriented the filter. In one case, a filter was accidentally placed upside down and had to be retrieved. In some cases, filters have been placed in the wrong blood vessel.
Failure, Breakage and Migration
Other complications relate to problems with the filter itself. For example, the filter might fail to completely open, it may tilt or be placed in the wrong location.
Sometimes, the filter may migrate to another location in your body. Some filters will fracture over time under normal repetitive stresses that naturally occur within your body.
IVC Filter Migration
Medical professionals consider a filter to have significantly migrated if it moves two centimeters or more from the initial location. This can happen for several reasons, including your vein being too large to accommodate the filter.
Overall, filter migration risk is estimated at less than 1%. Researchers say 90% of migration incidents happened more than 30 days after placement.
Migration into the cardiopulmonary system can be fatal, and it requires immediate intervention. This may include attempted percutaneous retrieval. If that is not feasible, then open-heart surgery is required.
Failure To Open
Sometimes the filter is defective and fails to open completely. This can also happen for other reasons, including an error on the part of the doctor who places the filter.
A 2016 study in the journal Cardiovascular Diagnosis & Therapy said this failure to open happens between 0.7% to 13.9% of the time. However, with the titanium Greenfield filter, it can happen in as many as 71% of cases. When this happens, the filter’s performance can be decreased by as much as 80%, especially for catching smaller clots.
Filter Fracture and Perforation
Filter fracture may occur early or late, depending on the filter type. However, it is usually seen in filters that have been in place for more than a year. Researchers have found that the filter may fatigue and fracture over time under normal repetitive stresses that occur naturally within your body.
Therefore, promptly removing filters after they are no longer needed can help you avoid this complication.
In one study, researchers evaluated 80 patients who had two particular brands of filters inserted between 2004 and 2009, the Bard Recovery and the Bard G2 filters. Roughly 16% of the patients had at least one of their filters’ struts fracture. In five cases, the strut had lodged in the patients’ hearts. Three of the patients had life-threatening conditions.
Sometimes the filter perforates your vein. This happens more often with retrievable filters that have been left in place longer than intended. Serious, but rare cases, have involved perforation of the duodenum, aorta and renal pelvis.
If a patient with a filter experiences non-specific abdominal or back pain, physicians should suspect possible filter component penetration.
Pain Related To Filter Complications
Pain experienced by patients with an IVC filter may be related to the filter. Some filter-related complications causing pain include IVC penetration, filter component embolization and a blocked filter resulting in severe leg pain.
Sometimes, a broken filter piece may cause pain where it lands, including the upper abdomen or chest. A filter penetration in one location may also cause referred pain in a region higher or lower than the original filter position. Therefore, pain associated with IVC filter complications can affect your chest, abdomen, pelvis and legs.
Abdominal or Back Pain from Perforation or Migration
Abdominal or back pain associated with an IVC filter is typically due to penetration through your blood vessel wall, impingement against nearby nerves or penetration into adjacent organs. Migration of filter components or referred pain may affect other areas of your body.
Perforation and migration account for about 22% and 20% of all reported complications, respectively.
A case report in 2016 involved a 49-year-old woman who suffered from severe abdominal pain and previous back pain. Her other symptoms included nausea, anorexia, non-bloody vomiting and diarrhea. A CT scan showed migration of all four struts of her IVC filter.
The struts had penetrated a nearby blood vessel (her aorta), part of her spine, muscle located adjacent to her lower spine and pelvic region, and tissues located between various organs and her abdominal wall.
Although open surgery was previously needed to remove IVC filters and repair patients’ injuries, newer minimally invasive techniques can now achieve retrieval in most patients without the need for invasive open surgery.
Leg Pain Related to Blockage
Leg pain from IVC filters is often due to a blockage. When several clots become trapped in the filter, clot formation down the IVC can cause painful, debilitating swelling in your legs.
Other signs and symptoms of a problem might include darkening of your skin and ulceration in your lower extremities.
Patients may have difficulty identifying the cause of their leg pain. Any pain that is severe or worsens suddenly should be immediately evaluated by a doctor, as it could represent new blood clots or DVT.
Detachment Risks to Heart and Lungs
When a filter strut breaks loose, makes its way through your bloodstream and enters your heart or lungs, it’s called embolization. You can suffer acute chest pain similar to a heart attack.
Adverse event reports submitted to the FDA between 2005 and 2010, included 146 reports of embolization out of 921 total reports.
Embolization of IVC filters to the heart and lungs can have serious and sometimes deadly consequences. Signs and symptoms of this condition might include acute chest pain, abnormal heart rhythm, shortness of breath, feeling faint and loss of consciousness.
A 2008 case study in the Texas Heart Institute Journal describes a 69-year-old patient who was implanted with an IVC filter which ended up moving to the right ventricle of his heart. His primary symptom was an abnormal life-threatening heart rhythm known as ventricular tachycardia.
After the device was removed, he developed a leaky tricuspid valve in his right heart chamber. His doctors believed the device had become entangled in the valve, which sustained damage when the device was removed.
In some cases, open heart surgery may be needed to remove the filter or repair damage caused by IVC filter embolization to the heart.
DVTs Related to IVC Filters
Patients with IVC filters have a risk of developing a blood clot in their lower-body vein known as deep vein thrombosis (DVT).
The risk of DVT doubles two years after a filter is placed. The incidence of this complication has been estimated to be as high as 43%.
Another possible complication is called caval thrombosis, or blood clotting in the vena cava. Rates of occurrence are estimated to range between 2% and 30%.
FDA Warnings and IVC Filter Recalls
The FDA first advised removing retrievable IVC filters once the pulmonary embolism risk subsides, citing severe complications like migration, fracture and perforation.
In 2014, the FDA issued its recommendation for a maximum implantation time of 29 to 54 days. The agency also required manufacturers to conduct studies, like the PRESERVE study, to address safety concerns regarding filters used in medical procedures.
Thousands of IVC Filters Recalled
Between 2005 and 2015, thousands of IVC filters were recalled. Two of the IVC filter recalls were Class I, which is the most serious designation the FDA can assign to a recall.
In December 2005, Boston Scientific issued a Class I 18,000 Greenfield IVC filters. The manufacturer said a defect could cause parts to separate while being implanted, which may cause cardiac or pulmonary embolism.
Boston Scientific also recalled two lots of filters for possible blood vessel damage in August 2005.
Cordis’s OptEase IVC filter had a Class I recall because of a labeling error that could cause the filter to be implanted backward. That recall affected 33,000 units.
Attention to complications may have contributed to the decline in the use of IVC filters. In 2013, 44,680 filters were implanted, compared to only 19,501 in 2019.
Lawsuits and Legal Action Against IVC Filter Manufacturers
Thousands of patients have filed lawsuits against IVC filter manufacturers like C.R. Bard and Cook Medical. These IVC filter lawsuits allege that the devices were defectively designed and caused serious injuries.
Lawsuits against C.R. Bard and Cook Medical were combined into multidistrict litigation (MDL). An MDL is when several similar lawsuits are consolidated into a single litigation to simplify and expedite the legal process.
As of May 2026, there were 6,562 Cook IVC filter lawsuits pending in MDL 2570 in a southern Indiana federal court.
C.R. Bard entered into negotiations to settle cases against it in an Arizona federal court. As of September 15, 2023, no C.R. Bard IVC filter lawsuits remained in the multidistrict litigation. MDL-2641 closed in July 2024.
Juries delivered verdicts against C.R. Bard and Cook Medical in state courts and bellwether trials. Bellwether trials are test cases that MDLs conduct to determine if plaintiffs have a case that may lead to settlements or dismissals of the MDL lawsuits.
| DATE | MANUFACTURER | PLAINTIFF VERDICT |
|---|---|---|
| May 2021 | C.R. Bard | An Oregon state jury awarded $926,000 to Justin Peterson in a state court trial after he claimed an IVC filter injured his small intestine. |
| August 2020 | C.R. Bard | The 9th Circuit upheld a $3.6 million jury award from 2018 to Sherr-Una Booker in an MDL bellwether trial. This was the only one of five bellwethers that a plaintiff won. |
| May 2018 | Cook Medical | A jury in a Texas state court awarded $1.2 million to Jeff Pavlock, who claimed an IVC filter damaged his aorta and small intestine. |
Cook Medical Hid IVC Filter Complications
A 2024 article in the Annals of Internal Medicine found hidden safety concerns and poor testing with Cook Medical’s Celect IVC filter.
Examining unsealed court records, researchers found the device was first denied FDA approval. However, it later received approval through the agency’s 510(k) authorization pathway.
Rather than proving a medical device is safe, a 510(k) allows for approval if the device is substantially similar to one already on the market.
“The Celect IVC filter case demonstrates the need for regulatory reforms to ensure that critical safety data are accessible to the FDA, clinicians and patients to inform decision making.”
The court document and public records review revealed that reports of complications and patient deaths submitted to the FDA omitted crucial details. Researchers also found these incidents were wrongly represented in published studies and on the Celect IVC label.
Consequently, patients and health care providers received misleading information about the device’s safety.
What To Do if You Experienced IVC Complications
If you had an IVC filter implanted, talk to your doctor about whether it should be removed. These filters are intended to be temporary. Keeping one in place for too long can lead to serious complications.
If you’re unsure about your filter’s status or you experience nausea, swelling, redness, fever or chest pain after implantation, consult your doctor immediately.
If you believe your filter has harmed you, consider speaking with a lawyer who specializes in medical device cases to discuss your options. Drugwatch can connect you with an experienced attorney for a free consultation.
Before talking to a lawyer, gather your medical records, including all information about your IVC filter procedure and any complications you were treated for following the procedure. Timely action can reduce your health risks and help you understand your rights if a device fails.
Calling this number connects you with a Drugwatch.com representative. We will direct you to one of our trusted legal partners for a free case review.
Drugwatch.com's trusted legal partners support the organization's mission to keep people safe from dangerous drugs and medical devices. For more information, visit our partners page.