Benicar
Benicar is a prescription blood pressure medication manufactured by Japanese drugmaker Daiichi Sankyo. Its active ingredient is olmesartan medoxomil, which is available as a generic formulation. The medication belongs to the angiotensin II receptor blocker (ARB) drug class and works by blocking the angiotensin II hormone, which causes blood vessel constriction and high blood pressure.
Our content is developed and backed by respected legal, medical and scientific experts. More than 30 contributors, including product liability attorneys and board-certified physicians, have reviewed our website to ensure it’s medically sound and legally accurate.
legal help when you need it most.
Drugwatch has provided people injured by harmful drugs and devices with reliable answers and experienced legal help since 2009. Brought to you by The Wilson Firm LLP, we've pursued justice for more than 20,000 families and secured $324 million in settlements and verdicts against negligent manufacturers.
More than 30 contributors, including mass tort attorneys and board-certified doctors, have reviewed our website and added their unique perspectives to ensure you get the most updated and highest quality information.
Drugwatch.com is AACI-certified as a trusted medical content website and is produced by lawyers, a patient advocate and award-winning journalists whose affiliations include the American Bar Association and the American Medical Writers Association.
About Drugwatch.com
- 17 Years of Advocacy
- $324 Million Recovered for Clients
- 20,000 Families Helped
- A+ BBB Rating
- 4.9 Stars from Google Reviews
Testimonials
I found Drugwatch to be very helpful with finding the right lawyers. We had the opportunity to share our story as well, so that more people can be aware of NEC. We are forever grateful for them.
- Medically reviewed by Rita Soni, Pharm.D., BCPS
- Last update: May 6, 2026
- Est. Read Time: 6 min read
The U.S. Food and Drug Administration (FDA) first approved brand-name Benicar in 2002 to treat high blood pressure. Then, in 2003, it approved Benicar HCT, a drug that contains both olmesartan and hydrochlorothiazide, a blood pressure medication from the thiazide diuretic drug class.
Millions of Americans use Benicar and its generics each year.
With over 7 million prescriptions, olmesartan was among the 100 most prescribed drugs in the United States in 2023, according to the U.S. Department of Health and Human Services’ most recent Medical Expenditure Panel Survey data.
What Does Benicar Treat?
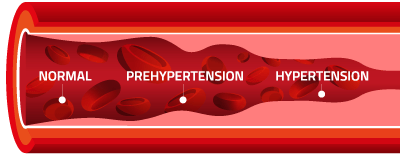
Doctors prescribe Benicar to treat hypertension, also known as high blood pressure.
Blood pressure rises as blood vessels constrict. While it’s normal for blood pressure to rise and fall throughout the day, health problems can develop for individuals whose blood pressure remains high for an extended period.
When left unchecked, elevated blood pressure levels greatly increase a person’s risk for heart disease and stroke, leading causes of death in the United States. High blood pressure usually has no accompanying symptoms, so many people are unaware that there’s even a problem.
For patients suffering from high blood pressure, taking a medication like Benicar can reduce the risk of heart attack and stroke.
Who Should Not Use Benicar?
Benicar can result in complications for fetuses, especially in the second and third trimesters, and some of these complications can be fatal to the fetus. Also, children under one year old should not take Benicar, as it can negatively affect the growth and development of the kidneys. Other individuals can also experience adverse reactions when taking Benicar.
Experts do not recommend Benicar for the following people:
- Children under one year of age
- Nursing mothers
- Patients with stiffening of renal arteries (also called renal artery stenosis)
- Pregnant women
Benicar Side Effects
The most common Benicar side effect is dizziness. Serious and less common side effects include facial edema (swelling of the face), high potassium levels (also known as hyperkalemia), low blood pressure (known as hypotension) and decreased kidney function.
Benicar can also cause some serious side effects, including potentially severe gastrointestinal issues and kidney injuries.
- Sprue-Like Enteropathy: 35.7%
- Gastroesophageal Reflux Disease: 20%
- Acute Kidney Injury: 15.2%
In 2013, the FDA released a safety announcement warning the public that Benicar has the potential to cause intestinal problems known as sprue-like enteropathy. Symptoms of drug-induced sprue-like enteropathy include severe, chronic diarrhea and substantial weight loss within months to years after beginning use of the medication.
Signs and Symptoms of Sprue-Like Enteropathy
- Abdominal pain
- Anemia
- Bloating
- Chronic diarrhea
- Fatigue
- Malabsorption
- Nausea/Vomiting
- Weight loss
Benicar is also toxic to developing fetuses and can result in fetal abnormalities or death.
Potential fetal abnormalities include skull abnormalities, low blood pressure and kidney failure. Some babies may be unable to produce and pass urine. These effects are most common during the second and third trimesters of pregnancy.
Patients should discontinue Benicar as soon as possible after detecting pregnancy.
- Back pain
- Blood in urine
- Bronchitis
- Diarrhea
- Elevated triglyceride levels (fat in the blood)
- Flu-like symptoms
- Headache
- High blood sugar
- Increase in creatinine phosphokinase (CPK)
- Mucous membrane inflammation
- Pharynx inflammation
- Sinusitis
Black Box Warning – Fetal Toxicity
A black box warning appears on a prescription drug’s label when the FDA wants to call attention to serious or life-threatening risks associated with its use. Benicar contains one of these warnings for fetal toxicity. The label says individuals should stop taking Benicar as soon as they realize they’re pregnant. This is because olmesartan acts directly on the renin-angiotensin system, which regulates blood pressure. As a result, fetuses can experience reduced kidney function, underdeveloped lungs, skeletal deformations and an increased risk of death. The label says the risks are greater during the second and third trimesters.
There are risks for newborn babies as well, including underdeveloped skulls, a lack of urine production, low blood pressure, kidney failure and premature death.
Drug Interactions With Benicar
It is possible for Benicar to cause adverse reactions when taken concurrently with certain drugs (both prescription and nonprescription). These adverse reactions may include unfavorable side effects and decreased effectiveness.
- Aliskiren (Brand Name – Tekturna):
- Experts recommend that patients with diabetes avoid taking Benicar in conjunction with the blood pressure medication aliskiren.
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs):
- Taking Benicar with NSAIDs, a type of pain medication including ibuprofen (Motrin) and naproxen (Aleve), can lead to decreased kidney function. Taking NSAIDs can also decrease the effects of Benicar.
- ACE Inhibitors and Angiotensin II Receptor Blockers:
- Taking Benicar with other ARBs or ACE inhibitors (such as captopril, ramipril, lisinopril, quinapril and others) is associated with increased risks of low blood pressure, high potassium and changes in kidney function.
- Colesevelam Hydrochloride (Brand Name – Welchol):
- Taking colesevelam hydrochloride with Benicar reduces the effectiveness of Benicar. Doctors recommend that patients take Benicar at least four hours before taking a dose of colesevelam hydrochloride in order to decrease the effect of the drugs’ interaction.
Mayo Clinic Study Confirms Olmesartan-Induced Enteropathy
Researchers monitored 22 patients who visited the Mayo Clinic between August 2008 and August 2011, examining the link between olmesartan and unexplained sprue-like enteropathy.
To be included in the study, patients had to have chronic diarrhea (lasting more than four weeks) while taking olmesartan. The cause of the symptoms could not be explained by another disorder, such as celiac disease. The final criterion was that discontinuing olmesartan resulted in clinical improvement regarding enteropathy symptoms.
Mayo Clinic’s 2012 Report
In 2012, Mayo Clinic researchers published this study as a case series of sprue-like enteropathy associated with patients’ use of olmesartan.
2012 Results:
- The 22 subjects involved in the series presented similar clinical results to adverse event reports identified by the FDA through its Adverse Event Report System (FAERS).
- Of the 22 patients from 17 states treated by the Mayo Clinic from 2008 to 2011, 14 required hospitalization with weight losses averaging almost 40 pounds, and one patient lost about 125 pounds.
- None of the patients responded to gluten-free diets (used for celiac disease sufferers).
- They were all taking daily doses of olmesartan ranging from 10 to 40 mg.
- When doctors discontinued olmesartan treatment, the patients’ symptoms improved, and they all experienced some degree of weight gain.
Mayo Clinic’s 2013 Report
In May 2013, researchers published an article in the American Journal of Gastroenterology describing patients with negative blood tests for celiac disease and villous atrophy, a condition in which the wall of the intestine erodes away.
2013 Results:
- The article reported that some patients without definitive causes for villous atrophy received diagnoses for unclassified sprue.
- Researchers later discovered that some of these patients had villous atrophy associated with their use of olmesartan.
Researchers further investigated olmesartan-induced enteropathy using prescription refill information and Medicare insurance claims, which showed that patients using olmesartan had a higher rate of celiac disease diagnoses than users of other ARBs.
One 2022 clinical study noted the potential of tiny olmesartan medoxomil particles delivered through the nose to improve the drug’s effectiveness. The engineered bioparticles showed a significant decrease in blood pressure and heart rate.
FDA-Initiated Label Change for Sprue-Like Enteropathy
In 2013, the FDA issued a safety announcement about the potential for occurrences of sprue-like enteropathy among patients taking Benicar. This decision came following its evaluation of adverse event reports, the Mayo Clinic case series and information from the Centers for Medicare and Medicaid Services (CMS) database. The FDA also ordered olmesartan manufacturers to include a warning about sprue-like enteropathy on drug labels.
In premarketing clinical trials, the incidence of olmesartan adverse effects reported by Daiichi Sankyo was similar to the placebo group. Dizziness was the only negative effect linked directly to olmesartan with greater frequency than the placebo. While millions of individuals have taken olmesartan over the years, reports of severe gastrointestinal reactions associated with its use didn’t surface until later in 2012.
Less than a year after the FDA ordered the label change for Benicar and other drugs containing olmesartan, patients who had suffered sprue-like enteropathy began filing Benicar lawsuits. Daiichi Sankyo, Benicar’s manufacturer, agreed in August 2017 to settle Benicar claims from about 2,300 plaintiffs for $300 million.
Warning Letter To Benicar Manufacturer
In 2006, the U.S. Department of Health & Human Services (HHS) submitted a warning letter to Sankyo Pharma Inc. The letter requested that Sankyo immediately cease its promotion of certain sales and marketing materials that contained unsubstantiated claims of effectiveness and superiority. HHS also alleged that Sankyo omitted or minimized information on the risks associated with the use of Benicar.
The omitted or minimized risk information included:
- Lithium interactions
- Renal artery stenosis (narrowing of arteries that carry blood to the kidneys)
- Serious pregnancy-related risks
- Warnings regarding the use of Benicar HCT in patients with impaired liver function or lupus
In addition to the marketing warnings, Daiichi Sankyo faced kickback allegations. The U.S. Justice Department accused Daiichi Sankyo of paying doctors to prescribe Benicar. Daiichi Sankyo paid $39 million to settle the case.
Calling this number connects you with a Drugwatch.com representative. We will direct you to one of our trusted legal partners for a free case review.
Drugwatch.com's trusted legal partners support the organization's mission to keep people safe from dangerous drugs and medical devices. For more information, visit our partners page.




