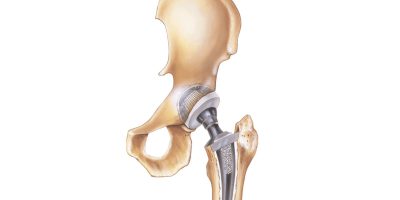
Hip Replacement Complications
Joint loosening, blood clots, change in leg length, dislocation, fractures and infection are common hip replacement complications. People who have received metal-on-metal hips may also experience metallosis, a form of metal poisoning that causes tissue damage and other serious conditions.
Our content is developed and backed by respected legal, medical and scientific experts. More than 30 contributors, including product liability attorneys and board-certified physicians, have reviewed our website to ensure it’s medically sound and legally accurate.
legal help when you need it most.
Drugwatch has provided people injured by harmful drugs and devices with reliable answers and experienced legal help since 2009. Brought to you by The Wilson Firm LLP, we've pursued justice for more than 20,000 families and secured $324 million in settlements and verdicts against negligent manufacturers.
More than 30 contributors, including mass tort attorneys and board-certified doctors, have reviewed our website and added their unique perspectives to ensure you get the most updated and highest quality information.
Drugwatch.com is AACI-certified as a trusted medical content website and is produced by lawyers, a patient advocate and award-winning journalists whose affiliations include the American Bar Association and the American Medical Writers Association.
About Drugwatch.com
- 17 Years of Advocacy
- $324 Million Recovered for Clients
- 20,000 Families Helped
- A+ BBB Rating
- 4.9 Stars from Google Reviews
Testimonials
I found Drugwatch to be very helpful with finding the right lawyers. We had the opportunity to share our story as well, so that more people can be aware of NEC. We are forever grateful for them.
- Medically reviewed by Chaitanya Dev Pannu, M.D.
- Last update: February 25, 2026
- Est. Read Time: 7 min read
Common Hip Replacement Complications and Risks
Hip replacement complications are rare. The most common symptoms that can sometimes occur include stiffness, pain, swelling and change in leg length. With appropriate rehabilitation and physiotherapy, most of these symptoms resolve over time.
One leg may feel longer after surgery because of the way the implant fits. Putting a lift in one shoe may correct this sensation.
- Bladder infection
- Blood clots and nerve damage
- Change in length
- Dislocation
- Fracture
- Infection
- Leg-length inequality
- Loosening or failure of device
- Muscle weakness
- Stiffness
- Swelling
- Tingling sensation
- Unexpected pain
Serious complications are even more rare, but can include bleeding, blood clots, blood vessel injury, dislocation, fractures, infection, implant loosening and nerve injury. Serious complications may require revision surgery. It is critical to manage risk factors such as obesity, smoking and diabetes to minimize these risks.
Hip replacement complications can happen during surgery. For example, during the implantation of the femoral stem, bone around the device can be fractured. These fractures are typically managed with additional screws, wires or surgical intervention. Other complications can develop weeks, months or even years after a typical recovery period.
Risk Factors for Hip Replacement Complications
Age and overall health factor into complication risks, Dr. H. John Cooper, an orthopedic surgeon at Columbia Doctors in New York, told Drugwatch. Diabetes, smoking, substance abuse and certain medications can affect the chance for complications.
“It can be somewhere between 0.3% for somebody who’s healthy and in good shape,” Dr. Cooper said. “There are risk factors that are greater than 20% in patients with the wrong sort of combination of risk factors.”
Complications from hip resurfacing and partial hip replacements, referred to as hemiarthroplasty, are generally the same as those from total hip replacements. Patients should talk to their surgeons about the most common risks associated with the type of hip surgery they will be undergoing.
“When problems do happen, they can be life-altering for patients,” Dr. Cooper noted.
Blood Clots and Nerve Damage
Nerves and blood vessels can sometimes be damaged during surgical procedures. In hip replacement surgery, damage can occur when the surgical team cuts through tissue and moves it out of the way to implant the artificial hip. Modern techniques such as nerve monitoring can help reduce these risks.
Blood clots are a common risk after any major surgery. To reduce the risk of clots traveling to the lungs or heart, surgeons often prescribe blood thinners like low-molecular-weight heparin or aspirin for a few weeks after surgery.
Component Loosening and Early Implant Failure
Loosening is a serious long-term complication and is an indicator that a revision surgery will be required. Components can loosen because they wear out or cement fails to hold them in place. While this is more common in older implant designs, newer cementless and hybrid implants have improved longevity.
A study published in Orthopedics looked at 80 patients with metal-on-metal (MoM) hips who needed revision surgery. The most common problem was the socket portion of the hip loosening without any infection.
Almost 57% of the patients in the study experienced this problem. Another 13% experienced soft tissue reactions, which can also result in loosening.
Dislocation After Hip Replacement and Revision Surgery
Dislocation occurs in about 2% of patients within the first year of hip replacement. The rate jumps to 28% in patients who undergo revision hip surgery, according to a study in the journal Deutsches Arzteblatt. The dislocation risk can be influenced by factors such as the surgical approach (anterior vs. posterior), implant design and patient activity levels.
Authors Jens Dargel and colleagues called dislocation “extremely traumatizing for patients,” and they warned that it could cause patients to lose confidence in the implant.
“The dislocation of a total hip [implant] is an emotionally traumatizing event that should be prevented if possible.”
“The dislocation of a total hip [implant] is an emotionally traumatizing event that should be prevented if possible,” the authors wrote.
Dargel and colleagues recommended surgeons work with patients to minimize the chances of dislocation.
Heterotopic Ossification
Only 2% – 7% of hip replacement patients present any symptoms of heterotopic ossification. Less than 1% require surgery as a result. Although it is usually asymptomatic, in severe cases it may require treatment such as nonsteroidal anti-inflammatory drugs (NSAIDs) or, in rare instances, surgical excision.
A review of previous studies in the Indian Journal of Orthopaedics found a probability of heterotopic ossification in more than 90% of patients who experienced the condition after a previous hip replacement surgery.
Heterotopic ossification occurs when bone grows in soft tissues such as muscle or tendons. This growth can be three times as fast as normal bone growth and can cause pain around an artificial hip because of its jagged edges.
Infection Is a Serious Risk Following Hip Replacement

The American Academy of Orthopaedic Surgeons puts the risk of postoperative infection at about 1%. If the infection is caught quickly, doctors may reopen the wound to clean it and inject antibiotics.
If that does not work or if the infection is not discovered until later, the implant may need to be removed and re-implanted after the infection has been eradicated.
“Most of our patients don’t tend to think joint infections cause death, and [infections] don’t immediately put people at risk for mortality,” Dr. Cooper told Drugwatch. “But if you look at the five-year mortality of somebody who gets a hip or knee infection, it’s worse than most cancers.”
“If you look at the five-year mortality of somebody who gets a hip or knee infection, it’s worse than most cancers.”
Long-Term Wear: Metallosis and Osteolysis
While hip implants may last 20 years or longer, they do wear out. The act of the ball moving in the socket releases microscopic particles with every movement.
Studies show that as many as 470,000 particles can be released in every step with a metal and polyethylene artificial hip. And anywhere from 5 to 250 million metal particles can be released with metal artificial hips.
In metal-on-metal hips, these particles over time can cause metallosis, a type of metal poisoning. In hip replacements with plastic parts, they can cause bone resorption called osteolysis. Particles can also cause tissue to break down or affect organs in the body.
Metallosis
The buildup of metallic debris in the soft tissue of the body causes metallosis, a rare and potentially fatal condition. It’s most often associated with metal-on-metal hip implants.
Metallosis causes tissue death around the artificial hip and leads to the implant loosening. It’s been at the center of several hip replacement lawsuits.
One study reported metallosis was diagnosed in 5% of metal-on-metal hip arthroplasties. Rates declined as the use of metal-on-metal implants declined.
Osteolysis
Osteolysis occurs when debris from the wear on artificial hip joints accumulates in surrounding tissue. The debris’ presence causes inflammation that destroys bone and loosens the hip implant.
Reports find bone loss following total hip replacement “remains a significant concern.” One Swedish study reported osteolysis accounted for more than 75% of revision surgeries in Sweden from 1979 to 2002.
Reviewing the study’s results, researchers noted, “The incidence of periprosthetic osteolysis in many studies is greater than the sum of all the rest of the complications.”
Periprosthetic Fractures
Periprosthetic fractures involve bone breaks around the implant that can cause it to fail. These fractures are rare and usually occur years after a hip replacement, according to the American Academy of Orthopaedic Surgeons.
A fall, direct blow to the hip or car crash can cause these fractures to occur. Osteoporosis and medicines that weaken bones can increase the risk for periprosthetic fractures.
Estimates of the frequency of periprosthetic fractures after replacement surgery are wide ranging – from 0.1% to 18%. The rates were 4% to 11% following revision surgery.
Death After Hip Replacement Surgery
Studies have found a decrease in mortality risk as hip arthroplasty techniques have become more sophisticated. A study in the U.K. reported death after hip arthroplasties in England and Wales decreased from 0.56% in 2003 to 0.29% in 2011.
In the U.S., 90-day mortality decreased from 1.2% in 1991 to 0.8% in 2008, according to a study in the Journal of the American Medical Association.
Research indicates that age, preexisting health conditions and overall fitness play a significant role in mortality risk. In one study, heart disease was responsible for 431 deaths within 90 days of total hip replacement surgery. The data also indicated an increase in digestive system-related deaths.
Calling this number connects you with a Drugwatch.com representative. We will direct you to one of our trusted legal partners for a free case review.
Drugwatch.com's trusted legal partners support the organization's mission to keep people safe from dangerous drugs and medical devices. For more information, visit our partners page.