Premarket Approval (PMA)
The most stringent approval process for medical devices is the U.S. Food and Drug Administration’s Premarket Approval, which is required for a relatively small percentage of devices that are deemed the most risky.
Our content is developed and backed by respected legal, medical and scientific experts. More than 30 contributors, including product liability attorneys and board-certified physicians, have reviewed our website to ensure it’s medically sound and legally accurate.
legal help when you need it most.
Drugwatch has provided people injured by harmful drugs and devices with reliable answers and experienced legal help since 2009. Brought to you by The Wilson Firm LLP, we've pursued justice for more than 20,000 families and secured $324 million in settlements and verdicts against negligent manufacturers.
More than 30 contributors, including mass tort attorneys and board-certified doctors, have reviewed our website and added their unique perspectives to ensure you get the most updated and highest quality information.
Drugwatch.com is AACI-certified as a trusted medical content website and is produced by lawyers, a patient advocate and award-winning journalists whose affiliations include the American Bar Association and the American Medical Writers Association.
About Drugwatch.com
- 17 Years of Advocacy
- $324 Million Recovered for Clients
- 20,000 Families Helped
- A+ BBB Rating
- 4.9 Stars from Google Reviews
Testimonials
I found Drugwatch to be very helpful with finding the right lawyers. We had the opportunity to share our story as well, so that more people can be aware of NEC. We are forever grateful for them.
- Medically reviewed by Mireille Hobeika, Pharm.D.
- Last update: December 11, 2025
- Est. Read Time: 8 min read
The FDA has regulated medical devices since 1976. The agency classifies medical devices based on the potential risk they pose. Class I devices are the least risky and include things like surgical tools and oxygen masks.
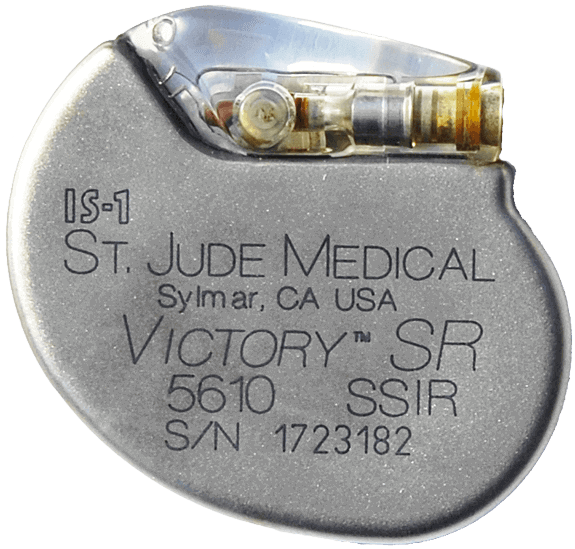
Medical devices that are listed as Class III are considered the most risky devices, determined to present a potential for serious risk to the health, safety or welfare of the patient. They include such things as replacement heart valves, pacemakers, and implanted cerebellar stimulators. Over time, depending on the development of scientific data, devices can change classification.
Although most Class III devices are subject to FDA’s Premarket Approval (PMA), there is an exception: Class III devices that were already on the market in 1976 or before the FDA was given authority in this area. These devices are not subject to PMA.
Class II devices are technically less risky than Class III devices, and are subject to a less-rigorous clearance process called 510(k) or Premarket Notification (PMN). Estimates are that 95 to 98 percent of devices come to the U.S. market through the 510(k) or premarket notification, while just 5 percent come to market over the tougher route, known as premarket approval or PMA.
In November 2022, the FDA reported it had approved 112 devices through the PMA process in October 2022 alone.
Rare and Costly Process
It costs a manufacturer an average of about $94 million to bring a medical device onto the market through PMA, compared to $31 million for the much less stringent 510(k) process. Part of the cost is in the form of a user fee from the FDA, with the standard fee for PMA set at nearly $235,000, compared to $4,690 for 510(k).
PMA requires extensive data from laboratory and clinical studies, which are not required under the more lenient 510(k) process.
But as rigorous as the PMA process is for device makers, it doesn’t compare to the amount of scrutiny the FDA gives to pharmaceuticals.
“It doesn’t make sense, if I want a prescription for constipation or diarrhea, why does it go through a more rigorous process than an artificial heart?”
Jeffrey Shuren, director of the Center for Devices and Radiological Health (CDRH), told Congress in March 2017 that the agency has made progress in shortening the amount of time it takes to grant 510(k) clearance. CDRH is the office at the FDA that regulates medical devices.
In 2009, Shuren noted, it took an average of 427 days to for a decision on PMA. By 2015, that average was 276 days, a decrease of 35 percent in six years.
In contrast, in 2015, it took an average of 133 days for the agency to reach a decision on 510(k) applications.
Pros and Cons for Device Makers
Manufacturers often prefer not to submit their devices to premarket approval, if they can avoid it, because of the time and expense. But one significant advantage to the companies who complete the process is it is also much more difficult for consumers to sue device makers for problems linked to medical devices that receive this stamp of approval from the FDA. That’s because the courts have applied a legal standard called preemption, which limits lawsuits in such circumstances. But the courts have held that preemption doesn’t apply to lawsuits involving devices that were cleared through 510(k), making it much easier to bring cases for injuries linked to those devices. Some manufacturers that can afford the expense also may see a competitive advantage to going the more difficult route, which may force other companies without the same resources to do the same and potentially keep the competition from the market.
Many manufacturers have used another process after receiving premarket approval that allows them to submit changes in devices with no requirement for clinical testing. A study of approvals for cardiac implantable electronic devices found that for every approved PMA, a mean of 50 supplements were approved. This study found that most new device models were deemed safe and effective without new clinical data.
The FDA review of an application for premarket approval is supposed to take six months — twice as long as 510(k) — but may, and usually does, take longer. In fact, in 2013, it took an average of 432 days to reach a decision. But the following year, it was 262 days. During that process, the device manufacturer is required to provide valid scientific evidence showing the safety and effectiveness of the device.
Research May Lack Needed Data
But as rigorous as the process is considered, manufacturers virtually always get the green light if they get over the first hurdle of persuading the FDA to accept and file their applications. According to one analysis, nearly every premarket approval application accepted by the agency in 2015 was granted — a 98 percent rate. As of March 2017, the rate was 100 percent, according to FDA data.
A little more than 6 percent of submitted applications were not accepted in the first half of fiscal year 2017. That was down 2 percentage points from the applications not accepted the prior year and more than an 11 percent reduction from the 17.6 percent of applications not accepted in 2013.
Critics say that PMA requires testing on a relatively small number of people on a short period of time. If the results demonstrate some benefits without major side effects, the FDA may approve the device.
And the studies used to justify the safety and effectiveness of medical devices have some shortcomings. In 2017, researchers at Yale and the University of California-San Francisco released the results of their own study that concluded that little of the research took into account such differences in patients as sex, age or race.
“We are learning so much about how sex and gender play a role in the development of diseases, conditions, and their treatments. It is time that we apply the same scrutiny to medical devices to ensure that they are safe and effective for all.”
Of 82 studies filed in 2015, just 4 percent included analysis by the race of patients and only 9 percent included analysis by age. Of the 77 studies that included both men and women, only 17 percent were analyzed by sex.
This was in spite of an action plan implemented by the FDA in 2014 calling for examination of results by age, race and ethnicity of patients.
Submitting an Application
The process starts when a manufacturer submits a detailed application to the FDA. This is described by the agency as a scientific, regulatory documentation to demonstrate to the FDA the safety and effectiveness of the device. The application also has to give details about how the device was designed and how it was manufactured.
The pre-market application Includes sections for:
- Technical information, which has data and other information to inform the agency’s decision whether to approve the application.
- Non-clinical laboratory studies, which gives information on microbiology, immunology, biocompatibility, stress, wear, shelf life, and other laboratory or animal tests. The FDA provides manufacturers guidance in how to conduct these appropriate studies.
- Clinical investigations, including details about how the studies were conducted, data about safety and effectiveness of the device, any adverse reactions and complications, failures and replacements of the device. This section also has information about patients, including complaints, data tabulations from all individual study subjects, and statistical analyses results.
The FDA also requires information about the labeling of the device. During the initial review stage, the FDA may ask the manufacturer for more information to go with an application. If the information isn’t provided by a set deadline, the application will be considered withdrawn and if the company wants to move forward, it must start the process all over.
If the FDA concludes the application doesn’t meet a minimum threshold of acceptability, it will not accept the application for further review. In that case, the agency will inform the submitter what is required for the application to be deemed acceptable. The applicant may resubmit the application with the additional information or may request an informal conference with an FDA official to review the decision not to accept the application. The director of the Center for Devices and Radiological Health’s decision will be considered the final word.
After the Application is Accepted
If, after the initial, limited scientific review, the FDA decides to accept or file the application, then it is subjected to an in-depth, scientific, regulatory and quality review, also known as a substantive review, by FDA personnel.
During that detailed review, the FDA may again notify the applicant of any information needed to complete the process. The applicant may seek information on the status of the application by requesting a meeting within 100 days of the FDA’s filing of the application. If the applicant submits an amendment to the application with significant new data — including information from studies or analyses of data — the review period may be extended by up to 180 days.
If the device is a first of its kind, the application may be referred to an outside panel of experts that serves as an advisory committee. Future applications for that type of medical device won’t be sent to an advisory committee once the FDA is satisfied it understands factors related to the safety and effectiveness of the device and that the agency has the ability to address issues.
Advisory committees are required to hold a public meeting to review the application in accordance with the law. The transcript of that public meeting is forwarded to the FDA. The advisory committee also must submit a report to the FDA with its recommendation and the basis for it.
As part of its review, the FDA will inspect the manufacturing process and audit the clinical study data.
Once the FDA grants approval, it’s standard for the agency to impose conditions, such as advertising and label requirements. Manufacturers are also required to submit reports notifying the FDA of any problems associated with the device, also known as adverse events.
Calling this number connects you with a Drugwatch.com representative. We will direct you to one of our trusted legal partners for a free case review.
Drugwatch.com's trusted legal partners support the organization's mission to keep people safe from dangerous drugs and medical devices. For more information, visit our partners page.




