Xarelto
Doctors prescribe Xarelto (rivaroxaban) to prevent blood clots and strokes. It requires no blood testing and is a once-a-day pill. However, the drug may cause internal bleeding that leads to hospitalization and death. In May 2018, the U.S. Food and Drug Administration approved the first antidote.
Our content is developed and backed by respected legal, medical and scientific experts. More than 30 contributors, including product liability attorneys and board-certified physicians, have reviewed our website to ensure it’s medically sound and legally accurate.
legal help when you need it most.
Drugwatch has provided people injured by harmful drugs and devices with reliable answers and experienced legal help since 2009. Brought to you by The Wilson Firm LLP, we've pursued justice for more than 20,000 families and secured $324 million in settlements and verdicts against negligent manufacturers.
More than 30 contributors, including mass tort attorneys and board-certified doctors, have reviewed our website and added their unique perspectives to ensure you get the most updated and highest quality information.
Drugwatch.com is AACI-certified as a trusted medical content website and is produced by lawyers, a patient advocate and award-winning journalists whose affiliations include the American Bar Association and the American Medical Writers Association.
About Drugwatch.com
- 17 Years of Advocacy
- $324 Million Recovered for Clients
- 20,000 Families Helped
- A+ BBB Rating
- 4.9 Stars from Google Reviews
Testimonials
I found Drugwatch to be very helpful with finding the right lawyers. We had the opportunity to share our story as well, so that more people can be aware of NEC. We are forever grateful for them.
- Medically reviewed by Kevin Lombardi, M.D., MPH
- Last update: May 8, 2026
- Est. Read Time: 21 min read
Xarelto is described as a “next-generation” blood thinner. The drug can help reduce the risk of developing blood clots. Blood clots can travel through the bloodstream to the brain and cause strokes.
The U.S. Food and Drug Administration (FDA) approved Xarelto in November 2011 to reduce the risk of stroke and systemic embolism in people with non-valvular atrial fibrillation. The common heart disorder affects more than 3 million Americans. It results in irregular heart rhythm and can lead to strokes.
The FDA approved Xarelto to treat deep vein thrombosis and pulmonary embolism in November 2012. The agency also approved the drug to reduce the risk of both conditions recurring.
As of 2022, doctors have written more than 13 million Xarelto prescriptions in the U.S.
Xarelto became the most-prescribed blood thinner in its class in the country.
But Xarelto can cause serious and sometimes deadly bleeding. Studies show Xarelto results in the same rate of adverse bleeding events as warfarin. Warfarin is an older version of a blood thinner.
Until recently, Xarelto had no approved antidote to reverse bleeding in patients. The FDA gave its approval for AndrexXa, the first and only antidote for Xarelto’s uncontrolled bleeding, in May 2018.
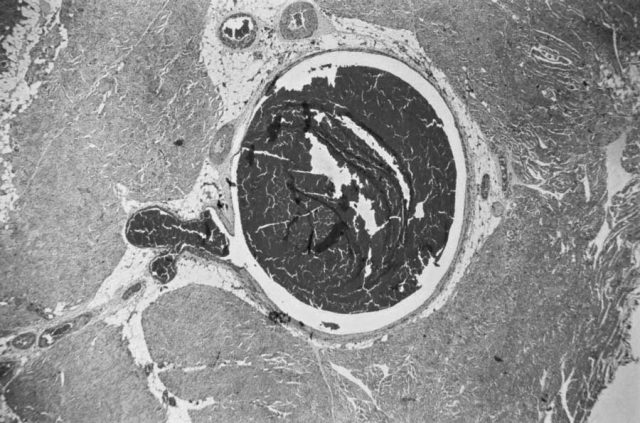
How Does Xarelto Work?
Xarelto (rivaroxaban) is a prescription blood-thinning medicine that targets Factor Xa (FXa), inhibiting its effect on the formation of blood clots in a patient’s arteries or veins. Factor Xa is the active form of Factor X, an enzyme that is synthesized in the liver and assists in coagulation, or clotting of the blood, changing it from a liquid to a gel.
Blood thinners like warfarin (brand name Coumadin) interfere with vitamin K’s ability to create blood clots in addition to impacting several other blood-clotting factors. Xarelto is considered a selective anticoagulant because it only interferes with one factor, Factor Xa, thereby interacting with fewer of the body’s natural functions.
Despite its categorization as a “blood thinner,” Xarelto and similar drugs do not actually thin a patient’s blood, so they cannot dissolve existing clots. But these medications can serve to prevent or reduce blood clotting and assist in preventing existing clots from growing larger and more dangerous.
What Does Xarelto Treat?
Xarelto (rivaroxaban) is indicated to reduce the risk of stroke and systemic embolism in patients with nonvalvular atrial fibrillation (an irregular heartbeat) by preventing the formation of blood clots. It is also used as a treatment and maintenance drug for deep vein thrombosis (DVT), a blood clot that forms in a vein deep in the body, usually in the lower leg or thigh. DVT may lead to a sudden blockage of an artery in the lung (pulmonary embolism, or PE) in patients having knee or hip replacement surgery.
Nonvalvular Atrial Fibrillation
Atrial fibrillation (AF) is the most common type of arrhythmia, or irregular heartbeat. If a patient has an arrhythmia, it means there is a problem with the speed or rhythm of their heartbeat. “Nonvalvular” means AF is not caused by a heart valve problem.
The cause of AF has to do with a disorder in the heart’s electrical system. A test called an electrocardiogram (EKG) can assist in the diagnosis of AF by showing the electrical waves of a patient’s heart. Complications of the condition can include an increased risk of stroke, chest pain, heart attack or heart failure, which can lead to death. Treatment of AF may include medications and/or other procedures designed to restore the heart’s normal rhythm.
Some patients with AF may not experience any signs of the disease.
- Heart palpitations
- Shortness of breath
- Weakness or difficulty exercising
- Chest pain
- Dizziness or fainting
- Fatigue
- Confusion
Deep Vein Thrombosis (DVT) and Pulmonary Embolism (PE)
Deep vein thrombosis (DVT) is a condition in which a blood clot forms in a vein deep within the body. DVT typically occurs in the large veins in the lower legs and thighs, but it can also occur in other deep veins, such as in the arms or pelvic region. If the vein swells, it is referred to as thrombophlebitis.
DVT is most common in individuals over 60. However, blood clots can occur at any age.
- Cancer
- Certain autoimmune disorders (including lupus)
- Certain medications, such as estrogens and birth control pills
- Cigarette smoking
- Fractures of the pelvis or legs
- Having a long-term catheter in a blood vessel
- Heart failure
- Obesity
- Personal or family history of DVT or PE
- Polycythemia vera (too many blood cells being made by the bone marrow)
- Pregnancy
- Prolonged bed rest, such as during a long hospital stay or paralysis
- Recent surgery (most commonly hip, knee or female pelvic surgery)
- Sitting still for a long time
Blood clots, including DVT, can affect blood flow. This may cause skin redness, leg pain or leg swelling (edema). It may also make a person’s skin feel warm or tender over the affected vein.
If a DVT breaks loose and travels through the bloodstream to the lung, it could cause a sudden blockage in an artery in the lung. This is called a pulmonary embolism (PE). PE can cause permanent damage to the affected lung, low blood oxygen levels and organ damage due to a lack of oxygen supply. If the clot is large or there are multiple clots present, PE can even result in death.
About 50% of individuals who have PE are unaware that they are affected by the potentially life-threatening condition. Symptoms can include shortness of breath, chest pain or coughing up blood. The goal of treatment is to break up any existing clots and to prevent new clots from forming.
Xarelto Side Effects
Common Xarelto side effects include minor bleeding, bruising, back pain, dizziness, headache, heavy periods, itching, tingling and nosebleeds. More serious side effects of Xarelto are major bleeding and epidural or spinal hematomas (a collection, or “pooling,” of blood outside the body’s blood vessels).
There is also an increased risk of thrombosis in patients who discontinue Xarelto. The drug carries a boxed warning for risks associated with blood clots and pooled bleeding.
Post-marketing reports also noted incidences of thrombocytopenia (blood platelet deficiency), hepatitis (liver inflammation) and a severe skin reaction called Stevens-Johnson syndrome.
Latest Side Effects Information
As of June 30, 2024, gastrointestinal bleeding was the most common Xarelto side effect reported to the FDA. There were also frequent reports of nosebleeds, blood in the urine, hemorrhage, stroke and DVT.
| FDA Adverse Events Reporting System (FAERS) Data for Xarelto Side Effects | |
|---|---|
| Total cases reported | 129,461 |
| Serious cases (including deaths) | 111,591 |
| Deaths | 20,372 |
FAERS data confirm study results showing that bleeding events are the most common side effects of Xarelto and similar drugs. The FDA considers the vast majority of reported adverse events as serious.
- Serious Side Effects: 86%
- Minor Side Effects: 14%
Common Xarelto Side Effects
According to prescribing information, bleeding is the most common side effect observed in adults taking Xarelto. Among pediatric patients, the most common side effects are bleeding, cough, vomiting and stomach or gut inflammation.
- Abdominal pain
- Back pain
- Bruising
- Difficulty breathing or swallowing
- Fatigue or tiredness
- Hives
- Lightheadedness
- Minor bleeding
- Muscle spasms
- Nausea and vomiting
- Pain in arms or legs
- Rash and itching
- Wound complications
Many Xarelto side effects are mild, resolve on their own and do not interfere with treatment. However, Xarelto has been linked to adverse bleeding events because blood thinners reduce clotting. Patients taking this medication are more likely to bruise easily, and it may take longer for bleeding to stop.
Data from clinical studies presented in the drug’s prescribing information show that Xarelto has an increased risk of major bleeding events compared to several other similar medications. This can cause serious health consequences, including death.
Managing Minor Bleeding
Minor bleeding is among the most common side effects of Xarelto. It can manifest as nosebleeds, heavier-than-normal periods, prolonged bleeding after a minor cut or bleeding gums. Some patients also report bruising more easily or bruises that fade slowly.
In general, minor bleeding is not a serious health threat and can be handled at home. Steps to help manage this side effect include applying pressure to cuts and using a soft toothbrush and waxed floss on teeth. Ice packs may help bruises fade more quickly. Pinching your nose and applying a cold compress can help stop nosebleeds
If any bleeding becomes excessive, discuss your options with your health care provider.
- Unexpected bleeding or bleeding that lasts a long time
- Bleeding that is severe and cannot be controlled
- Red, pink or brown urine
- Bright red or black stools that look like tar
- Coughing up blood or blood clots
- Vomiting blood or vomiting that resembles “coffee grounds”
- Headaches, dizziness or weakness
- Pain, swelling or new drainage at wound sites
Serious Xarelto Side Effects
Major bleeding is the most common serious side effect for patients taking Xarelto. Other serious side effects linked to rivaroxaban, the active ingredient of Xarelto, include anaphylaxis and hematomas.
- Allergic reactions
- Major bleeding
- Spinal and epidural hematomas
“Patients should monitor for signs and symptoms of major bleeding, including blood in the urine, blood in the stool, severe bruising, prolonged nosebleeds, and vomiting blood,” clinical pharmacist Kenneth S. Fill told Drugwatch.
Major bleeding events require immediate action. A 2024 study published in Fundamental & Clinical Pharmacology showed that both specific reversal agents that were designed as antidotes and nonspecific treatments, such as activated charcoal, can serve as antidotes to bleeding caused by direct oral anticoagulants.
However, as with other direct oral anticoagulants, discontinuing Xarelto may lead to an increased risk of developing thrombosis. Therefore, the discontinuation of Xarelto should be done with a health care provider’s guidance.
Abnormally High Risk of Internal Bleeding
Xarelto carries an abnormally high risk of internal bleeding. Taking Xarelto with certain other medications, including some common over-the-counter medications like NSAIDs (non-steroidal anti-inflammatory drugs) and aspirin, may increase this possibility.
Patients with a history of cancer, bleeding disorders, lung disease, lung cavities or bleeding in or around the lungs also face a greater risk of severe bleeding when taking Xarelto.
"Xarelto can cause bleeding, which can be serious and may lead to death… During treatment with Xarelto, you are likely to bruise more easily, and it may take longer for bleeding to stop."
Xarelto packaging contains a warning about the risk of serious and potentially fatal bleeding.
Multiple patients have filed Xarelto lawsuits against the manufacturers Janssen Pharmaceuticals and Bayer Corp. These lawsuits largely claimed the companies failed to fully warn patients about the medication’s risks. Many of the plaintiffs had experienced complications from serious internal bleeding while taking Xarelto. Others focused on wound leakage and infection after hip and knee replacement surgery.
Post-Surgical Wound Drainage and Infection
A 2021 study published in the British Journal of Clinical Pharmacology showed that patients taking rivaroxaban, the active ingredient in Xarelto, have a higher incidence of major or clinically relevant bleeding events after surgery than patients taking other types of medication.
Additionally, patients taking Xarelto have a higher incidence of post-surgical wound complications compared to those not using the medication. Infections and wound drainage may contribute to the need for additional surgery on the affected joint.
Boxed Warnings and Precautions
Initial labeling for Xarelto, as a part of its FDA approval in 2011, included two “black box warnings.” Black box warnings indicate that the drug could cause particularly dangerous side effects. The warnings have remained throughout numerous label changes.
The first warning advises patients taking Xarelto not to prematurely discontinue its use, as doing so may result in an increased risk of adverse thrombotic events. The manufacturer of the blood thinner also notes that in clinical trials involving patients with AF, an increased risk of stroke has been observed when individuals switch from Xarelto to warfarin. The label directs that if use of the anticoagulant medication is discontinued for a reason other than bleeding or end of treatment, patients should strongly consider the use of another blood thinner in Xarelto’s place.
"Epidural or spinal hematomas have occurred in patients treated with Xarelto who are receiving neuraxial anesthesia or undergoing spinal puncture. These hematomas may result in long-term or permanent paralysis."
The second black box warning advises patients of the potential for epidural or spinal hematomas to develop in individuals receiving neuraxial anesthesia (such as an epidural) or undergoing a spinal puncture. The warning further states that these hematomas can result in long-term or permanent paralysis, and that patients at risk should be routinely monitored for signs and symptoms of neurological impairment.
These side effects can cause severe, permanent health complications or death.
“[The boxed warning] emphasizes the need for careful monitoring of patients who are on Xarelto and are about to undergo a spinal puncture or epidural anesthesia, given the risk of spinal hematomas,” Fill told us.
The label also points to bleeding as a serious side effect, which can even lead to death. Taking certain medications, including NSAIDs, aspirin and certain antidepressants, like selective serotonin reuptake inhibitors (SSRIs) or serotonin norepinephrine reuptake inhibitors (SNRIs), while on Xarelto can increase a patient’s risk for bleeding.
New Antidote for Bleeding
In May 2018, Portola Pharmaceuticals was given the go-ahead to market AndrexXa for patients taking drugs like Xarelto and Eliquis who experience uncontrolled bleeding. Portola estimates that 90,000 people are admitted to hospitals in the U.S. every year because of bleeding from taking such medications, and AndrexXa is the only “antidote” for bleeding with this cause.
In early 2015, the FDA designated Andexxa “a breakthrough therapy.”
This means early evidence indicated that it was representative of “a substantial improvement” over existing therapies. It also means the drug would assist in the acceleration of the development and review of other drugs for serious or life-threatening conditions.
However, in August 2016, the FDA announced it would not approve AndrexXa. The agency said it needed more data.
But a year later, in August 2017, the FDA accepted Portola’s newly submitted application. In December 2017, Portola announced the FDA had extended its time to review the application until May 2018.
FDA Investigates Faulty Clinical Trial
In 2016, questions surfaced regarding the validity of the clinical trial, titled ROCKET-AF, largely used in the approval of Xarelto by the FDA. The agency launched an investigation into the matter following the July 2016 recall of a device called the Alere INRatio, used to monitor warfarin therapy in the control group of the study. The FDA acknowledged that the ROCKET-AF clinical trial “provided the primary data to support the 2011 approval of the blood thinner drug Xarelto (rivaroxaban).”
The device used to test for blood clotting during the ROCKET-AF clinical trials was recalled due to its propensity to provide falsely low results. CBS News reported that the manufacturer of the faulty device confirmed that “the problem dated back to 2002.”
Even though studies showed that there was no significant difference between warfarin and Xarelto in the risk of major bleeding (although bleeding in the brain and fatal bleeding were less common for patients taking Xarelto), the fear was that the device’s flaw could have skewed those results, making Xarelto seem like the safer choice compared to warfarin when that might not be the reality.
However, following the completion of what the FDA described as “a variety of analyses to assess the impact that this faulty monitoring device had on the ROCKET-AF study results,” the agency determined that the effects on strokes and bleeding, including bleeding in the head, were minimal in patients taking Xarelto. The agency further concluded that “Xarelto is a safe and effective alternative to warfarin in patients with atrial fibrillation.”
In October 2017, Bayer and Janssen announced they were halting another clinical study into the effectiveness and safety of Xarelto for the secondary prevention of stroke and systemic embolism in patients with a recent embolic stroke of undetermined source. The phase III clinical study ended early because it showed no better results than treatment with low-dose aspirin.
Administration and Dosing Information
Xarelto comes in three different dosage forms and strengths, including 10-, 15- and 20-milligram tablets. The 10- and 15-milligram tablets are both round and red, with the weaker strength exhibiting a lighter red hue. The 20-milligram tablets are triangle-shaped and dark red.
For patients with AF, Xarelto is typically taken once a day with an evening meal. A patient taking Xarelto for the treatment of AF should never stop taking the medication without first talking to their doctor, as that can increase the risk of the individual having a stroke or forming blood clots in other parts of the body.
The recommended dose of Xarelto for the treatment of DVT and/or PE is 15 mg taken orally twice daily with food for the first 21 days. After this initial treatment period, the recommended dose of Xarelto is 20 mg taken orally once daily with food, at approximately the same time each day.
The recommended dose of Xarelto for the reduction in the risk of recurrence of DVT or PE is 20 mg taken orally once daily with food at approximately the same time each day.
In patients taking Xarelto for the prevention of DVT, which could result in PE following certain surgical procedures, the recommended daily dose is generally 10 milligrams taken once a day, with or without food. The initial dose should be taken at six to 10 hours after surgery, once the patient has been stabilized or their body functions have returned to normal.
Patients taking Xarelto should generally continue treatment with the drug for 35 days following a hip replacement surgery. For patients undergoing knee replacement surgery, Xarelto should typically be continued for 12 days following the procedure. A patient’s doctor will ultimately decide how long a patient should continue to take Xarelto following surgery.
Sometimes, a patient’s doctor may ask them to stop taking Xarelto for a short time prior to certain surgeries or medical or dental procedures. The doctor will also inform the patient when it is considered safe to resume treatment with the blood thinner medication.
Overdose
It is possible to overdose on Xarelto (rivaroxaban) by consuming large amounts of the drug. If an overdose is suspected, patients are urged to seek immediate treatment, as potentially life-threatening bleeding complications can occur. Due to Xarelto’s high plasma protein binding, the drug is not dialyzable, meaning dialysis cannot be used to remove the medication from the patient’s blood. Since there is currently no specific antidote generally available to reverse bleeding in patients taking Xarelto, activated charcoal may be used to reduce absorption of the drug.
Mild cases of overdose may not result in any symptoms. Since there is currently no easy or overall effective way to treat a Xarelto overdose that results in bleeding, treatment is likely to be largely symptomatic and supportive, minimizing complications that occur rather than preventing them.
- Vision or speech changes
- Vomiting blood
- Severe headache
- Weakness or numbness in an arm or leg (this may be a sign of bleeding in the brain)
- Easy bruising
- Black, tarry stools or bright red blood in the stool (this may be a sign of gastrointestinal bleeding)
Dental Procedures and Xarelto
Due to concerns related to bleeding risks, it is sometimes suggested that patients discontinue the use of Xarelto prior to undergoing certain dental procedures. However, patients may also be told to adjust the timing of their Xarelto dosages around a surgery, or they may be told to take their medication as usual. Only you and your medical providers can make the right decision for your situation.
Another narrative issued the same year confirmed the advice offered by the first narrative author, but also addressed the need to consider other supplements or drugs the patient may be taking together with Xarelto that could increase the patient’s risk for bleeding and resultant complications.
With the inclusion of a 2013 systematic review as well, the overall recommendation was to advise patients not to take Xarelto one to three hours prior to dental treatment. All of the authors acknowledged that no clinical studies or guidelines have been published to directly address the treatment management considerations of patients taking Xarelto while undergoing various dental procedures, so any recommendations made are purely subjective.
The general consensus, according to the American Dental Association (ADA), seems to be that with the newer target-specific anticoagulant medications, no change to the treatment regimen is required for patients undergoing dental treatments. But the ADA suggested that in order to be cautious, dental practitioners should consult a patient’s physician to assess the safety for each individual patient, and that when suggesting any modification to a patient’s medication regimen prior to dental surgery, that it be done in conjunction with consultation of the patient’s primary care doctor.
Drug Interactions and Contraindications
Certain prescription and nonprescription medications, as well as certain vitamins and herbal supplements, may interact with Xarelto. Some could cause it to be less effective, while others may increase a patient’s risk for dangerous bleeding events and other side effects.
- Nizoral (ketoconazole)
- Antifungal medication used to treat infections caused by fungi
- Onmel, Sporanox (itraconazole)
- Used to treat fungal or yeast infections
- Norvir (ritonavir)
- A drug prescribed for the treatment of HIV in combination with other medications
- Kaletra (lopinavir/ritonavir)
- An antiretroviral fixed-dose combination drug used to treat and prevent HIV/AIDS
- Crixivan (indinavir)
- Prescribed for the treatment of HIV
- Carbatrol, Equetro, Tegretol, Tegretol-XR, Teril, Epitol (carbamazepine)
- Anticonvulsant medication used to treat seizures, nerve pain and bipolar disorder
- Dilantin-125, Dilantin (phenytoin)
- Used to treat seizures
- Solfoton (phenobarbital)
- A medication used to control epilepsy and seizures long-term
- Rifater, Rifamate, Rimactane, Rifadin (rifampin)
- This medication eliminates bacteria that cause tuberculosis (TB)
- St. John’s wort (Hypericum perforatum)
- Herbal supplement used to treat a variety of health conditions, now most commonly used for depression
Taking Xarelto along with painkillers, such as aspirin and NSAIDs, or other anticoagulants, can increase a patient’s risk of bleeding.
Xarelto is also contraindicated, meaning not advisable, for use by patients with active bleeding conditions or severe hypersensitivity (allergic reaction, such as anaphylaxis) to Xarelto (rivaroxaban) or any of its other ingredients.
Xarelto In Certain Populations
Certain individuals considering taking Xarelto may be at an increased risk of resulting complications. These individuals can include patients who have ever had bleeding problems, liver or kidney problems, or other medical conditions.
The drug’s overall safety and efficacy have not been adequately studied in pregnant women, and dosing for pregnant women has not yet been established. Women with high-risk pregnancies may be at an increased risk of bleeding and premature delivery. In animal studies, maternal bleeding and maternal and fetal death occurred during labor and delivery at a dose of 40 milligrams/kg of Xarelto. Therefore, Xarelto should be used during pregnancy only if the potential benefit justifies the potential risk to the mother and fetus.
The safety and effectiveness of Xarelto use in children have not yet been established.
Other Blood Thinners
Xarelto prevents clotting, so suddenly stopping the medication may cause excessive clotting. This can lead to thrombosis, which could lead to stroke or death.
If you must stop taking Xarelto, only do so after consulting your health care provider. You may need to switch to another anticoagulant to limit the risk of a clotting event.
Pradaxa (dabigatran) and Eliquis (apixaban) are direct oral anticoagulants, as is Xarelto. These blood thinners typically cause side effects similar to those seen with Xarelto.
Warfarin is an older kind of blood thinner that blocks the body’s ability to synthesize Vitamin K for blood clotting purposes. Therefore, you may need to modify your diet when taking warfarin to moderate your Vitamin K intake.
Lovenox, Fragmin and Arixtra are low-molecular-weight heparin (LMWH) medications. Similar to Xarelto, they work by blocking Factor Xa, an enzyme used for blood clotting. They have similar rates of wound complications compared to Xarelto.
“Xarelto’s risk of major bleeding compared to other DOACs such as apixaban, dabigatran, and edoxaban is similar, except when it comes to gastrointestinal bleeding, which is slightly higher,” Fill said. “It is important to note that the risk of bleeding can vary depending on patient factors.”

Warfarin, marketed under the brand names Coumadin and Jantoven, has been the primary anticoagulant (blood thinner) drug available to patients since its approval. However, since 2010, the FDA has approved additional oral anticoagulant drugs, including Pradaxa, Xarelto, Eliquis and Savaysa (edoxaban).
All four of those anticoagulants work to effectively reduce a patient’s overall risk of stroke associated with AF. But they can also cause bleeding, and only two of the blood thinners (warfarin and Pradaxa) currently have antidotes available to reverse this adverse effect.
The FDA concluded that all four anticoagulants in the new generation of blood thinners are equivalent to, or more effective than, warfarin in preventing strokes. Still, the availability of an antidote may be a game-changer for some patients when considering which medication to take.
Other benefits of this new wave of blood thinners over the tried-and-true warfarin include fewer interactions with food and other drugs, a more rapid onset, freedom from the need to undergo periodic blood testing, and a substantially reduced risk of bleeding into the brain resulting in hemorrhagic stroke (a type of stroke that is not caused by blood clots that go into the brain, such as those found in AF patients).
Calling this number connects you with a Drugwatch.com representative. We will direct you to one of our trusted legal partners for a free case review.
Drugwatch.com's trusted legal partners support the organization's mission to keep people safe from dangerous drugs and medical devices. For more information, visit our partners page.